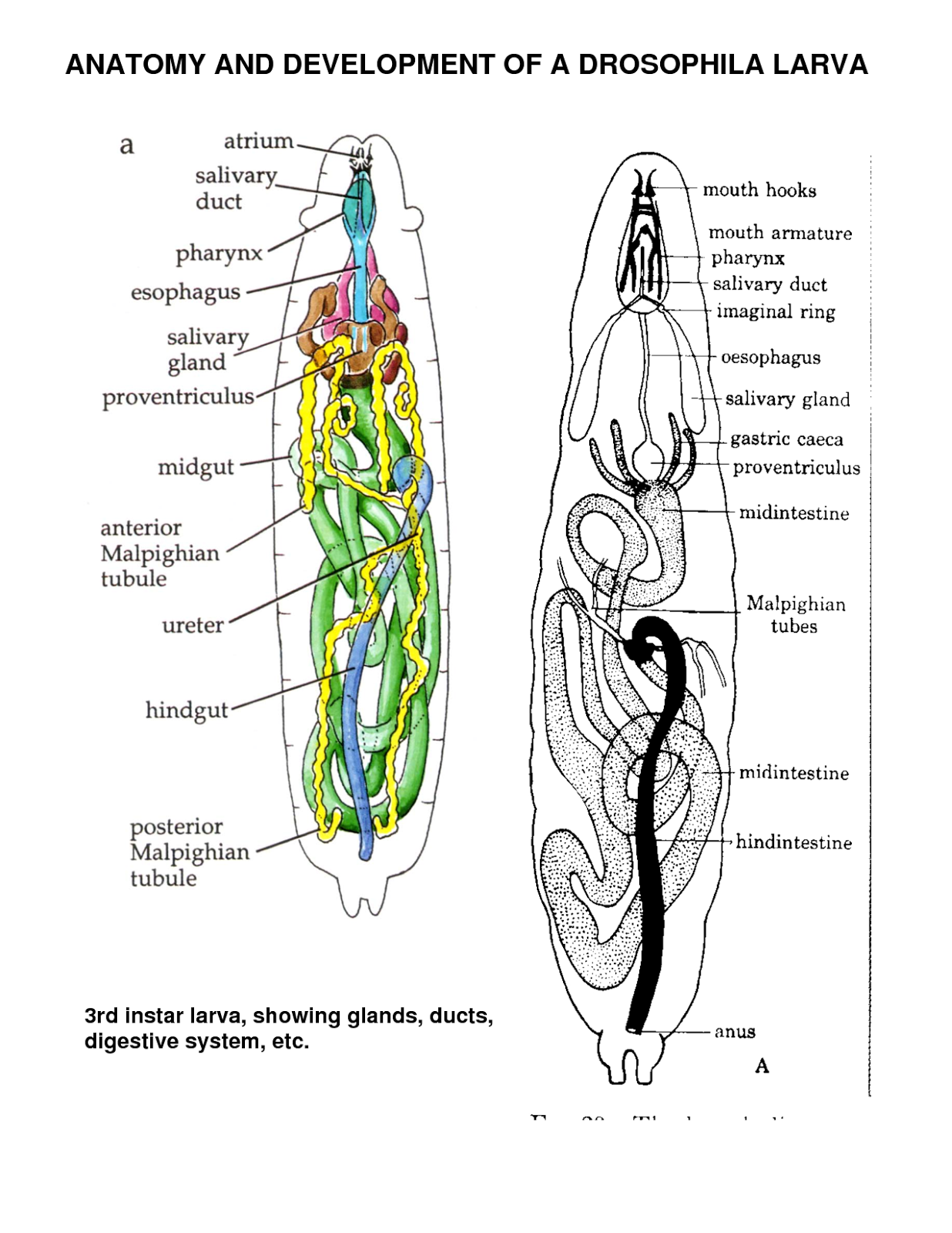
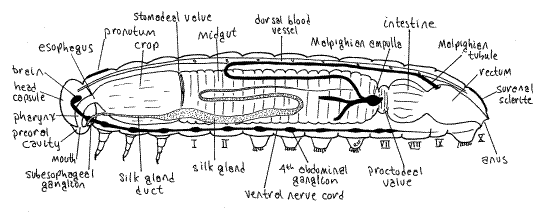
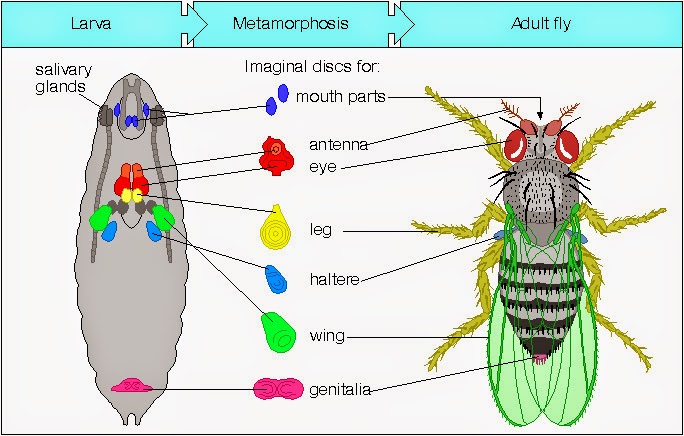
Venous eczema
This is the best solution I have ever found when a venous eczema is not responding to radiofrequency treatment; or when a skin graft is not taking:
The DFZ regime
Fucibet 30g x4tubes daily for 2/52
Zip Zoc bandage x14 apply daily
Dermal lotion 500 apply regularly to skin
Excellent results indeed!!
Interesting vascular history
Wiliam and John Hunter …
Scottish brothers … born in 1718 and 1728; William was a dedicated educated person .. John never enjoyed books but was fund of natural observations … William established anatomy school .. John joined in … and under William’s guidance, john became a professional anatomist and teacher …
John Hunter is well known for popliteal aneurysm repair. Potts noticed by that time that no matter how judiciously performed, proximal and distal ligation of aneurysm would not save the patient’s life. However, John realised that ligating very distally might be able to preserve the collaterals; hence his famous operation, published in London Medical Journal 1786. he decided to approach medially (not posteriorly). He did at St George’s Hospital.
Hunter’s pupils were numerous, including Astley Cooper.
However, his curiosity lead him to inoculate his own penis with a specimen taken from a patient suffering from urethritis. Years later, he developed syphilis and a syphilitic ascending aortic aneurysm.
He then was informed about the appointment of a predecessor in St George’s hospital; he suffered a major angina which proved fatal.
first vein graft –
Alfred Exner from Austria (used canine external jugular vein) then Alexis Carrel from France (University of Lyon). They published their revolutionary idea of using vein as a bypass in 1906 (Surgery, Gyn, and Obst).
Carrel designed the technique, that is still in use now:
A rigid asepsis is absolutely essential for success. . . . The dissection of the vessel is not dangerous if the wall of the vessel is not crushed or roughly handled with metallic forceps of other hard instruments . . . it is necessary that these clamps [vascular] be smooth-jawed and not too strong in the spring . . . by using very sharp, rough needles, only extremely small wounds are made . . . great care is taken not to include fragments of the connective tissue layer in the line of suturing, and to obtain a smooth union and approximation of the endothelial coats.
First clinical anastomosis, however, is sone/published by Jose Guyanese from Madrid. He used an adjacent popliteal vein piece to repair a popliteal aneurysm.
to be continued …
Scottish brothers … born in 1718 and 1728; William was a dedicated educated person .. John never enjoyed books but was fund of natural observations … William established anatomy school .. John joined in … and under William’s guidance, john became a professional anatomist and teacher …
John Hunter is well known for popliteal aneurysm repair. Potts noticed by that time that no matter how judiciously performed, proximal and distal ligation of aneurysm would not save the patient’s life. However, John realised that ligating very distally might be able to preserve the collaterals; hence his famous operation, published in London Medical Journal 1786. he decided to approach medially (not posteriorly). He did at St George’s Hospital.
Hunter’s pupils were numerous, including Astley Cooper.
However, his curiosity lead him to inoculate his own penis with a specimen taken from a patient suffering from urethritis. Years later, he developed syphilis and a syphilitic ascending aortic aneurysm.
He then was informed about the appointment of a predecessor in St George’s hospital; he suffered a major angina which proved fatal.
first vein graft –
Alfred Exner from Austria (used canine external jugular vein) then Alexis Carrel from France (University of Lyon). They published their revolutionary idea of using vein as a bypass in 1906 (Surgery, Gyn, and Obst).
Carrel designed the technique, that is still in use now:
A rigid asepsis is absolutely essential for success. . . . The dissection of the vessel is not dangerous if the wall of the vessel is not crushed or roughly handled with metallic forceps of other hard instruments . . . it is necessary that these clamps [vascular] be smooth-jawed and not too strong in the spring . . . by using very sharp, rough needles, only extremely small wounds are made . . . great care is taken not to include fragments of the connective tissue layer in the line of suturing, and to obtain a smooth union and approximation of the endothelial coats.
First clinical anastomosis, however, is sone/published by Jose Guyanese from Madrid. He used an adjacent popliteal vein piece to repair a popliteal aneurysm.
to be continued …
Bone marrow cell therapy (BMCT) – compared to distal ‘high risk’ bypass
ref. JVS 2015
Bone marrow aspirate injection for treatment of critical limb ischemia with comparison to patients undergoing high-risk bypass grafts
Kristina A. Giles, MD, Eva M. Rzucidlo, MD, Philip P. Goodney, MD, MS, Daniel B. Walsh, MD, Richard J. Powell, MD
outcome are really good ones, and certainly deserve trying in very high risk patients (like the guy I know about) ..
Shunting of carotid artery during CEA: is it useful or harmful
Ref: JVS Jan 2015
The impact of intraoperative shunting on early neurologic outcomes after carotid endarterectomy
Kyla M. Bennett, MD, John E. Scarborough, MD, Mitchell W. Cox, MD, Cynthia K. Shortell, MD
Interesting to see the results:
There was no significant difference in the incidence of postoperative stroke/TIA between the two groups of this matched cohort (3.4% in the no-shunt group vs 3.7% in the shunt group; P = .64).
Analysis of a similarly well matched subgroup of patients with severe stenosis or occlusion of the contralateral carotid artery demonstrated a statistically nonsignificant increase in the incidence of postoperative stroke/TIA with the use of intraoperative shunting (4.9% in the no-shunt group vs 9.8% in the shunt group; P = .08).
My experience in no shunting has been good enough (no postoperative stroke so far)… however, the anaesthetist struggled [seriously] to control the BP where a contralateral stenosis existed .. making me ‘think’ that using a shunt makes life better for the anaesthetist (and patient) in the BP control, no more, no less …
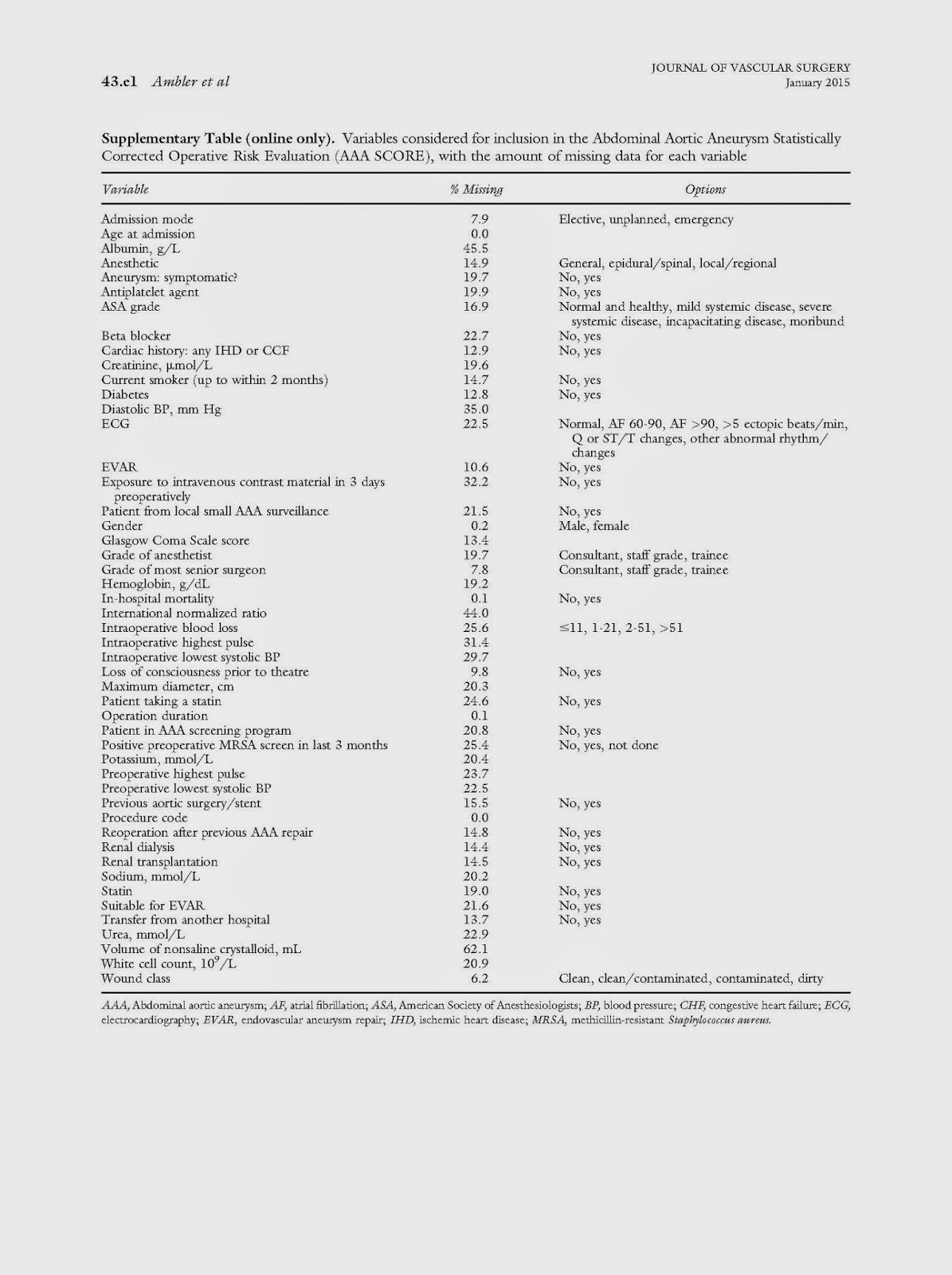
AAA SCORE
Ref. JVS Jan 2015
The Abdominal Aortic Aneurysm Statistically Corrected Operative Risk Evaluation (AAA SCORE) for predicting mortality after open and endovascular interventions
This is a good work aiming at predicting outcome following AAA surgery. The number of parameters used is large (49) but probably should anyway be available in any good quality vascular database.
The Score:
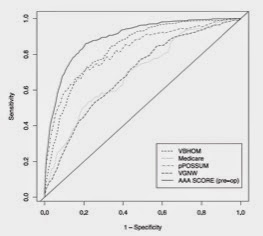
the calibration of this against other predictive models is shown in ROC curve:
This is quite good scoring system.. the main issue lies in the ability to apply it to practice; plus the cases were missing values exist … and of course how much this is going to add to the decision making …
It is also not unreasonable to say that the more factors you use, the better prediction you get … but practical life does not allow that … also, there are certain factors (duration of operation, wound class, etc.) that cn only obtained AFTER operating, not before … all make a scoring system like this not usable in decision making, but rather in (maybe) validating the performance of a unit/surgeon against others, after adjusting to risk (using the score). This is an important part of any quality assurance program in fact, and have certainly a role in current AAA practice.
What explains the persistent increase in aneurysm following a ‘sealed off’ Type I endoleak?
ref: EJVES Volume 49, Issue 1, January 2015, Pages 104
Re: ‘“Spontaneous Delayed Sealing in Selected Patients With a Primary Type Ia Endoleak After Endovascular Aneurysm Repair.” Does Correcting the Picture Save the Life?’
In the original paper (1), All but one of the 15 primary type Ia endoleaks sealed spontaneously within 5 months. The disappearance of type Ia endoleaks resulted from improved graft wall apposition due to neck remodelling or thrombosis of the non-apposed neck segment.
However, although ruptures were not detected in the 14 patients, sac growth occurred in four (28.5%).1 In these patients known causes of sac growth were not detected by CT.
Biomechanical explanation (which does make sense indeed) is that If the barrier between the aneurysm sac and the systemic arterial circulation consists of thrombus only, systemic pressure can be transmitted through a clot, and it is known that mural thrombus on the surface of the aneurysm sac does not prevent rupture.(2) For this reason, a thrombotic barrier on the neck segment may eliminate type Ia endoleak but may not prevent rupture.
Solution – Maybe by introducing a stiff barrier that prevent from transferring the pressure down into the sac. Feng et al.3 documented results of patients treated by fibrin glue injection: one aneurysm related death and four aneurysm sac growths were detected in 48 cases during 45 months follow up.
_________________________________________
- 1) F.B. Gonçalvez, H.J.M. Verhagen, K. Vasanthananthan, H.J.A. Zandvoort, F.L. Moll, J.A. van Herwaarden
-
Spontaneous delayed sealing in selected patients with a primary type Ia endoleak after endovascular aneurysm repairEur J Vasc Endovasc Surg, 48 (2014), pp. 53–59
- 2) F.J. Veith, R.A. Baum, T. Ohki, M. Amor, M. Adiseshiah, J.D. Blankensteijn, et al.
-
Nature and significance of endoleaks and endotension: summary of opinions expressed at an international conference
-
J Vasc Surg, 35 (2002), pp. 1029–1035
- 3) J.X. Feng, Q.S. Lu, Z.P. Jing, Y. Yang, B. Nie, J.M. Bao, et al.
-
Fibrin glue embolization treating intra-operative type I endoleak of endovascular repair of abdominal aortic aneurysm: long-term result
-
Zhonghua Wai Ke Za Zhi, 49 (10) (2011), pp. 883–887